Arizona's Vision Eye Care Center
Keratoconus is a progressive eye condition where the cornea thins and bulges into a cone shape, distorting vision in ways that glasses alone often cannot fully correct. It affects roughly 1 in 2,000 people, though recent screening studies suggest the true number may be higher. For patients and families in Phoenix navigating a new diagnosis, understanding what keratoconus is, how it progresses, and what treatments are available can make the difference between anxiety and confidence.
This guide covers everything you need to know. From the earliest warning signs and the diagnostic tools your eye doctor uses, to the full range of treatment options, the roles of optometrists and ophthalmologists in your care, and practical strategies for daily life with KC. Whether you are a patient, a parent of a teenager with changing vision, or a caregiver helping someone manage this condition, this resource is designed to give you clear, trustworthy answers.
What Is Keratoconus?
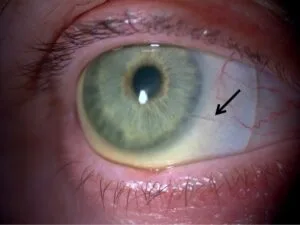
Keratoconus is a condition of the cornea, the clear, dome-shaped front surface of the eye. The word itself comes from the Greek “kerato” (cornea) and “conus” (cone), describing exactly what happens: the cornea gradually loses its round shape and begins to bulge outward. This structural change scatters light as it enters the eye, creating blurred and distorted vision that worsens over time if left unmanaged.
Keratoconus is not an infection. It is not caused by screen time or reading in dim light. It is a structural and biomechanical condition, and it typically appears during the teenage years or early twenties, progressing at different rates for different people.
How the Cornea Works in Healthy Vision
The cornea is responsible for about two-thirds of the eye's total focusing power. Think of it as the eye's front window. When light passes through a smooth, evenly curved cornea, it bends precisely onto the retina at the back of the eye, producing a sharp image. The cornea works together with the lens behind it to fine-tune focus at different distances.
A healthy cornea maintains its shape through a network of collagen fibers arranged in organized layers. These fibers give the cornea both its transparency and its structural strength. When this collagen framework is intact, the cornea holds its dome shape and refracts light predictably.
What Happens to the Cornea in Keratoconus
In keratoconus, the collagen cross-links that hold the cornea's structure together weaken. The tissue thins, most often at the lower center of the cornea, and begins to protrude forward into an irregular, cone-like shape. This irregular curvature means light no longer focuses cleanly on the retina. Instead, it scatters.
The result is progressive visual distortion. Straight lines may appear wavy. Multiple ghost images can overlap. Night vision often deteriorates significantly. Because the corneal surface becomes irregular, standard glasses and soft contact lenses lose their ability to correct vision effectively, since they sit on top of the distorted surface rather than compensating for it.
What Causes Keratoconus and Who Is at Risk?
Researchers have not identified a single definitive cause of keratoconus. Current evidence points to a combination of genetic predisposition, environmental triggers, and biomechanical factors that together weaken the corneal structure over time.
Known Causes and Contributing Factors
The most widely supported contributing factors include:
- Genetic factors. Keratoconus runs in families. Studies show that first-degree relatives of someone with KC have a 15 to 67 times higher risk of developing the condition compared to the general population. Multiple genes involved in collagen structure and oxidative stress response have been implicated.
- Oxidative stress and enzyme imbalance. Healthy corneas contain antioxidant enzymes that protect against free radical damage. In keratoconus corneas, researchers have found reduced levels of these protective enzymes, allowing oxidative damage to degrade collagen fibers.
- Chronic eye rubbing. Vigorous, habitual eye rubbing is one of the strongest modifiable risk factors. The mechanical force applied to the cornea during rubbing can accelerate thinning and distortion, particularly in corneas already predisposed to weakness.
- Inflammatory mediators. Although keratoconus was historically classified as a non-inflammatory condition, newer research has identified elevated levels of inflammatory markers in the tears and corneal tissue of KC patients, suggesting a low-grade inflammatory component.
Risk Factors for Developing Keratoconus
Certain populations and conditions carry higher risk:
- Age. Onset most commonly occurs between ages 10 and 25. Progression tends to be most rapid during the teenage years and often stabilizes by the mid-30s to 40s.
- Family history. Having a parent or sibling with keratoconus significantly increases risk.
- Allergic conditions. Eczema, asthma, and allergic conjunctivitis are associated with higher KC rates, partly because these conditions increase eye rubbing.
- Down syndrome. Individuals with Down syndrome have a keratoconus prevalence estimated at up to 15%, far exceeding the general population rate.
- Connective tissue disorders. Conditions like Ehlers-Danlos syndrome and Marfan syndrome, which affect collagen throughout the body, are associated with increased keratoconus risk.
- Hispanic and Middle Eastern heritage. Some population studies suggest higher prevalence in these groups, though research is ongoing.
Living in a hot, dry climate like Phoenix may also contribute to chronic eye irritation and rubbing, making awareness especially important for patients in the Valley.
Signs and Symptoms of Keratoconus
Keratoconus symptoms develop gradually. In the earliest stages, many patients assume they simply need a new glasses prescription. Recognizing the pattern of symptoms early can lead to faster diagnosis and better outcomes.
Early Warning Signs
The first signs of keratoconus are often subtle and easy to dismiss:
- Slightly blurred vision that does not fully correct with new glasses
- Increased sensitivity to light and glare
- Mild eye strain or headaches, especially after reading or screen use
- Frequent changes in eyeglass prescription, particularly increasing astigmatism
- Slight ghosting or shadowing around letters and objects
Many patients visit their optometrist multiple times for prescription updates before keratoconus is suspected. A pattern of rapidly changing astigmatism in a young patient is one of the most important clinical red flags.
Symptoms in Advanced Stages
As the cornea continues to thin and steepen, symptoms become more pronounced:
- Significant blurring and distortion that glasses cannot correct
- Streaking and flaring around lights, especially at night
- Double or multiple ghost images in one eye (monocular diplopia)
- Difficulty with night driving
- Halos around light sources
- In rare cases, acute hydrops, a sudden swelling of the cornea caused by a break in the inner corneal layer (Descemet's membrane), which causes sudden pain, tearing, and a dramatic drop in vision
If you or your child experience any combination of these symptoms, particularly worsening astigmatism with blurred vision that glasses do not fix, schedule a comprehensive eye exam promptly.
How Is Keratoconus Diagnosed?
Diagnosing keratoconus requires more than a standard vision test. While a routine eye exam can raise suspicion, confirming the diagnosis and tracking progression depends on specialized corneal imaging technology.
Comprehensive Eye Exam and Refraction Testing
The diagnostic process typically begins with a comprehensive eye exam. Your optometrist will measure your visual acuity, assess your refractive error (nearsightedness, farsightedness, astigmatism), and examine the overall health of your eyes.
During refraction testing, certain patterns raise suspicion for keratoconus. Irregular astigmatism that does not correct well with standard lenses, a scissoring reflex during retinoscopy, and rapidly shifting prescriptions are all clinical clues. Your doctor may also notice thinning or a cone-shaped protrusion when examining the cornea with a slit lamp microscope.
Corneal Topography and Tomography
The gold standard for keratoconus diagnosis is corneal topography, a non-invasive imaging test that maps the curvature of the corneal surface in precise detail. The test takes only seconds. You look at a target while the instrument projects rings of light onto your cornea and captures the reflected pattern.
A normal topography map shows a smooth, symmetrical curvature. A keratoconus map reveals characteristic patterns: inferior steepening, asymmetric bow-tie patterns, or a localized area of high curvature corresponding to the cone.
Corneal tomography, such as Pentacam or Orbscan imaging, goes further by measuring the back surface of the cornea and corneal thickness (pachymetry) across the entire cornea. This is critical because early keratoconus often shows changes on the posterior corneal surface before the front surface becomes obviously abnormal. Tomography can detect subclinical keratoconus, sometimes called “forme fruste” keratoconus, before symptoms develop.
Why Early Detection Matters
Early detection changes the trajectory of keratoconus care. When KC is caught in its early stages, corneal cross-linking can be performed to halt or significantly slow progression, potentially preventing the need for more invasive treatments later.
This is why routine comprehensive eye exams are so important, especially for teenagers and young adults with a family history of keratoconus or a pattern of increasing astigmatism. An optometrist equipped with corneal topography can identify keratoconus years before it becomes visually debilitating.
Keratoconus Stages and Classification
Keratoconus is typically classified into stages based on corneal curvature (measured in diopters), corneal thickness, and the degree of visual impairment. Understanding where you fall on this spectrum helps guide treatment decisions.
Mild Keratoconus
In mild keratoconus, corneal curvature readings are below approximately 45 diopters. The cornea shows early thinning and slight irregular astigmatism, but vision can often still be corrected to functional levels with glasses or soft toric contact lenses. Corneal topography reveals early asymmetric steepening, but the cone is not yet prominent.
Many patients at this stage are unaware they have keratoconus. Their primary complaint is usually that their glasses prescription keeps changing.
Moderate Keratoconus
Moderate keratoconus involves corneal curvature readings between approximately 45 and 52 diopters. The cornea is noticeably thinner, and the cone shape is more defined. Vision with glasses becomes inadequate, and most patients at this stage require specialty contact lenses, such as rigid gas permeable (RGP) or scleral lenses, to achieve clear vision.
Corneal scarring may begin to develop at this stage, particularly if the patient has a history of vigorous eye rubbing. Slit lamp examination may reveal Vogt's striae (fine stress lines in the cornea) or a Fleischer ring (an iron deposit ring around the base of the cone).
Advanced Keratoconus
Advanced keratoconus is characterized by corneal curvature readings exceeding 52 diopters, significant corneal thinning (often below 400 microns), and prominent scarring. Contact lens fitting becomes increasingly difficult. Visual acuity, even with specialty lenses, may be limited by scarring.
At this stage, surgical options such as corneal transplant may be considered if contact lenses can no longer provide functional vision. Acute hydrops, though uncommon, is most likely to occur in advanced disease.
Treatment Options for Keratoconus
Keratoconus treatment is not one-size-fits-all. The right approach depends on the stage of the disease, the rate of progression, and the patient's visual needs. Treatment goals are twofold: correct the vision distortion caused by the irregular cornea, and stop or slow the progression of the disease itself.
Glasses and Soft Contact Lenses (Early Stage)
In the earliest stages of keratoconus, standard eyeglasses or soft toric contact lenses may provide adequate vision correction. Soft torics can mask mild amounts of regular astigmatism, and many patients function well with these options initially.
However, as the corneal irregularity increases, soft lenses conform to the distorted corneal shape rather than correcting it. Patients typically notice that their vision with soft lenses becomes progressively less sharp, prompting the need for specialty lens options.
Rigid Gas Permeable (RGP) and Scleral Lenses
Specialty contact lenses are the cornerstone of keratoconus vision correction for moderate and many advanced cases.
Rigid gas permeable (RGP) lenses are small, firm lenses that vault over the irregular cornea, creating a smooth optical surface. The tear film that fills the gap between the lens and the cornea acts as a liquid lens, neutralizing much of the corneal irregularity. RGP lenses provide significantly sharper vision than soft lenses for KC patients, though some patients find them less comfortable initially.
Scleral lenses are larger diameter gas permeable lenses that rest on the white part of the eye (the sclera) rather than directly on the cornea. They vault completely over the cornea, creating a fluid-filled reservoir that bathes the corneal surface. Scleral lenses offer several advantages for keratoconus patients:
- Superior comfort compared to smaller RGP lenses
- Stable fit even on highly irregular corneas
- Continuous hydration of the corneal surface
- Excellent visual acuity
Scleral lenses have become the preferred contact lens option for many keratoconus patients. Fitting these lenses requires specialized expertise, and your optometrist may use digital corneal mapping to design a custom lens that matches your unique corneal shape.
Hybrid lenses combine a rigid center with a soft skirt, offering a middle ground between RGP sharpness and soft lens comfort. Piggyback systems, where a soft lens is worn beneath an RGP lens, are another option for patients who struggle with RGP comfort.
Corneal Cross-Linking (CXL)
Corneal cross-linking is the only treatment proven to slow or halt the progression of keratoconus. It does not reverse existing corneal changes, but it strengthens the collagen bonds within the cornea to prevent further thinning and bulging.
The procedure involves applying riboflavin (vitamin B2) drops to the cornea and then exposing it to controlled ultraviolet-A (UVA) light. This combination triggers a photochemical reaction that creates new cross-links between collagen fibers, stiffening the corneal tissue.
The FDA approved corneal cross-linking in 2016 for progressive keratoconus in the United States. Two main approaches exist:
- Epithelium-off (epi-off) CXL: The outer layer of the cornea (epithelium) is removed to allow better riboflavin absorption. This is the most studied and widely used technique.
- Epithelium-on (epi-on) CXL: The epithelium is left intact, resulting in less discomfort and faster recovery, though historically with somewhat less consistent results. Newer protocols and formulations are improving epi-on outcomes.
Recovery from epi-off CXL typically involves several days of discomfort, light sensitivity, and blurred vision, with visual stabilization occurring over weeks to months. The procedure is most effective when performed early in the disease, before significant scarring or thinning has occurred.
Cross-linking is particularly important for younger patients, whose keratoconus is more likely to progress rapidly. If your eye doctor identifies progression, a timely referral for CXL evaluation can preserve corneal integrity and reduce the likelihood of needing a transplant in the future.
Intacs Corneal Implants
Intacs are small, clear, crescent-shaped plastic inserts that are placed within the corneal tissue to flatten the cone and improve the corneal shape. They do not cure keratoconus, but they can reduce the degree of irregular astigmatism, potentially improving vision with glasses or contact lenses and making contact lens fitting easier.
Intacs are typically considered for patients with moderate keratoconus who are contact lens intolerant or who have difficulty achieving adequate vision with lenses alone. The procedure is reversible. The implants can be removed or exchanged if needed.
Intacs are sometimes combined with corneal cross-linking to both reshape and stabilize the cornea in a single treatment plan.
Corneal Transplant Surgery
Corneal transplant, or keratoplasty, is reserved for advanced keratoconus cases where contact lenses no longer provide functional vision or where significant corneal scarring blocks light from entering the eye. Approximately 10 to 20% of keratoconus patients eventually require a corneal transplant.
Two main types of transplant are used for keratoconus:
- Penetrating keratoplasty (PK): A full-thickness corneal transplant where the entire central cornea is replaced with donor tissue. PK has a long track record and high success rates for keratoconus, with graft survival rates exceeding 90% at 10 years.
- Deep anterior lamellar keratoplasty (DALK): A partial-thickness transplant that replaces the front layers of the cornea while preserving the patient's own inner endothelial layer. DALK reduces the risk of endothelial rejection and may offer better long-term graft survival, though it is technically more demanding.
Recovery from corneal transplant takes months. Sutures remain in place for a year or longer. Most transplant patients still require glasses or contact lenses after surgery to achieve their best vision, since the transplanted cornea may have some residual astigmatism.
The good news is that with earlier diagnosis and the availability of corneal cross-linking, the rate of transplants for keratoconus has been declining.
Optometrist vs. Ophthalmologist: Who Manages Keratoconus Care?
One of the most common questions patients and families have after a keratoconus diagnosis is: “Who should I be seeing for this?” The answer is often both an optometrist and an ophthalmologist, working together at different stages of your care.
The Role of Your Optometrist in Keratoconus
Your optometrist is typically the first eye care professional to detect keratoconus. Through comprehensive eye exams, corneal topography, and careful refraction, optometrists identify the condition, monitor its progression, and manage the primary vision correction.
For most keratoconus patients, the optometrist serves as the ongoing primary provider. Key responsibilities include:
- Performing corneal topography and tomography to track changes over time
- Fitting and managing specialty contact lenses (scleral, RGP, hybrid)
- Monitoring for signs of progression that may warrant a referral
- Coordinating care with ophthalmology when surgical intervention is needed
- Providing education and support for daily management
Optometrists with experience in keratoconus and specialty lens fitting are essential to achieving the best possible vision and comfort. Not all contact lenses are created equal, and the difference between a well-fitted scleral lens and a poorly fitted one can be dramatic.
When You Need an Ophthalmologist or Corneal Specialist
Ophthalmologists, specifically corneal specialists, become involved when keratoconus requires surgical or procedural intervention. You may be referred to an ophthalmologist for:
- Corneal cross-linking to halt progression
- Intacs implantation to reshape the cornea
- Corneal transplant evaluation and surgery
- Management of acute hydrops or other complications
- Co-management of complex cases where both medical and surgical expertise is needed
A corneal specialist is an ophthalmologist who has completed additional fellowship training focused on diseases and surgery of the cornea. For keratoconus patients facing surgical decisions, this subspecialty expertise is important.
How Coordinated Care Works at Arizona's Vision Eye Care Center
At Arizona's Vision Eye Care Center, we believe keratoconus care works best when your providers communicate and collaborate. Our optometrists perform the detailed diagnostic imaging, specialty contact lens fitting, and ongoing monitoring that form the foundation of KC management. When progression is detected or surgical options need to be explored, we coordinate directly with trusted corneal specialists in the Phoenix area to ensure a seamless transition.
This means you do not have to navigate the system alone. We handle referrals, share imaging and clinical records, and stay involved in your care before, during, and after any procedures. Our goal is to make sure you always know what is happening, why, and what comes next.
Living with Keratoconus: Daily Life and Long-Term Management
A keratoconus diagnosis can feel overwhelming, especially for younger patients and their families. But with proper management, most people with KC lead full, active lives with functional vision. Understanding how to protect your eyes and manage the condition day to day makes a real difference.
Protecting Your Eyes and Slowing Progression
The single most important thing you can do to protect your corneas is to stop rubbing your eyes. This cannot be overstated. Chronic eye rubbing is strongly associated with keratoconus progression, and eliminating this habit is a critical part of management.
Practical strategies include:
- Treat underlying allergies aggressively. If itchy eyes are driving the rubbing, work with your eye doctor to manage allergies with antihistamine drops, cold compresses, or oral medications. In Phoenix, seasonal allergens and dry desert air can make this especially challenging.
- Use preservative-free artificial tears. Keeping the ocular surface lubricated reduces irritation and the urge to rub.
- Wear UV-protective sunglasses outdoors. UV exposure and wind can irritate the eyes. Quality wraparound sunglasses help, particularly in the intense Arizona sun.
- Attend all scheduled follow-up appointments. Regular corneal topography monitoring allows your doctor to detect progression early and intervene with cross-linking before significant damage occurs.
- Follow your contact lens care routine precisely. Proper lens hygiene prevents infections and complications that could worsen corneal health.
Emotional and Practical Coping Strategies
Being told you have a progressive eye condition, especially during adolescence or young adulthood, can trigger anxiety about the future. Will my vision keep getting worse? Will I need surgery? Can I still drive?
These concerns are valid, and addressing them is part of good care. Here are some things to keep in mind:
- Keratoconus is manageable. The vast majority of patients maintain functional vision throughout their lives with appropriate treatment. Corneal cross-linking has changed the outlook dramatically by offering a way to halt progression.
- You are not alone. Online communities and support groups, such as the National Keratoconus Foundation and KC-focused forums, connect patients and families with others who understand the experience.
- Communication with your eye care team matters. If your lenses are uncomfortable, if your vision is not meeting your needs, or if you are struggling emotionally, tell your doctor. Adjustments can almost always be made.
- Plan ahead for practical needs. Keep a backup pair of glasses even if they do not provide perfect vision. Carry lens supplies when traveling. Discuss driving vision requirements with your optometrist.
Keratoconus in Children and Teens
Keratoconus often begins during puberty, and it tends to progress more aggressively in younger patients. Parents should be alert to signs such as:
- Frequent squinting or head tilting
- Complaints of blurry vision despite recent glasses
- Difficulty seeing the board at school
- Rubbing eyes excessively, especially if the child has allergies or eczema
- Rapidly changing prescriptions at annual eye exams
If your child is diagnosed with keratoconus, early intervention with corneal cross-linking is especially important. The younger the patient, the more years of potential progression lie ahead, and stabilizing the cornea early preserves the most options for long-term vision correction.
Fitting children and teens with scleral lenses requires patience and a skilled practitioner, but most young patients adapt well. Involving them in their own care, explaining what is happening in age-appropriate terms, and maintaining a positive, solution-focused outlook helps them manage the condition with confidence.
Keratoconus Care in Phoenix, AZ
Phoenix's unique environment creates specific considerations for keratoconus patients. The dry desert climate, intense UV exposure, high pollen counts during certain seasons, and dust can all contribute to eye irritation and the urge to rub. Awareness of these local factors is an important part of managing KC in the Valley.
Finding the Right Eye Care Provider in Phoenix
When choosing an eye care provider for keratoconus in Phoenix, look for:
- Corneal topography and tomography on-site. Your provider should have the imaging technology needed to diagnose and monitor KC accurately.
- Experience with specialty contact lens fitting. Scleral lens fitting for keratoconus is a specialized skill. Ask about the provider's experience with KC patients specifically.
- Established referral relationships with corneal specialists. If you need cross-linking or surgery, your optometrist should have direct relationships with fellowship-trained corneal surgeons in the Phoenix metro area.
- A collaborative care philosophy. The best outcomes happen when your optometrist and ophthalmologist work as a team, sharing records and communicating about your progress.
What to Expect at Your First Keratoconus Appointment
If you suspect keratoconus or have been referred for evaluation, here is what a thorough first appointment typically includes:
Your doctor will review your symptoms, vision history, and family history. A comprehensive eye exam will assess your visual acuity and refractive error. Corneal topography and, ideally, tomography will be performed to map the shape and thickness of your cornea in detail.
Based on the findings, your doctor will explain whether keratoconus is present, what stage it is in, and whether there are signs of recent progression. You will discuss vision correction options, whether cross-linking should be considered, and what the monitoring schedule should look like going forward.
Bring your current glasses and any contact lenses you wear. If you have records from a previous eye care provider, bring those as well. Write down your questions beforehand. A good first appointment should leave you feeling informed, not overwhelmed.
Conclusion
Keratoconus is a progressive corneal condition, but it is not a diagnosis without answers. From early detection through corneal topography to vision correction with scleral lenses and disease stabilization with corneal cross-linking, today's patients have more effective options than ever before. Understanding the stages, symptoms, and treatment pathways puts you in control of your eye health.
The key to the best possible outcome is timely, coordinated care. An experienced optometrist who can detect keratoconus early, fit specialty lenses precisely, and coordinate with corneal specialists when needed gives you the strongest foundation for long-term vision. Whether you are a patient, a parent, or a caregiver, knowing what to expect at each stage reduces uncertainty and builds confidence.
At Arizona's Vision Eye Care Center, we guide keratoconus patients through every step, from initial diagnosis and specialty lens fitting to referrals for cross-linking and surgical co-management. If you or someone in your family is experiencing changing vision, increasing astigmatism, or has been told they may have keratoconus, contact our Phoenix office to schedule a comprehensive evaluation. We are here to help you see clearly and move forward with confidence.
Frequently Asked Questions About Keratoconus
Can keratoconus cause blindness?
Keratoconus very rarely causes complete blindness. Even in advanced cases, vision can usually be restored through specialty contact lenses or corneal transplant surgery. The condition causes significant visual distortion, but with proper management, functional vision is maintained in the vast majority of patients.
Is keratoconus hereditary?
Keratoconus has a genetic component. If a parent or sibling has the condition, your risk is significantly higher than the general population. However, keratoconus does not follow a simple inheritance pattern, and many patients have no known family history.
What age does keratoconus usually start?
Keratoconus most commonly appears between the ages of 10 and 25. It tends to progress most rapidly during the teenage years and often stabilizes by the mid-30s to early 40s, though this varies from person to person.
Can rubbing your eyes cause keratoconus?
Chronic, vigorous eye rubbing is strongly associated with keratoconus development and progression. While rubbing alone may not cause KC in every case, it is considered a significant modifiable risk factor. Stopping the habit is one of the most important things patients can do.
Does corneal cross-linking hurt?
During the procedure, numbing drops are used, so most patients feel little to no pain. After epithelium-off cross-linking, patients typically experience discomfort, light sensitivity, and tearing for several days as the surface heals. Pain is usually manageable with prescribed medications and improves steadily.
Can you wear regular contact lenses with keratoconus?
In the earliest stages, soft contact lenses or glasses may still provide acceptable vision. As the condition progresses and the cornea becomes more irregular, standard soft lenses cannot correct the distortion effectively. Most keratoconus patients eventually need specialty lenses such as scleral or rigid gas permeable lenses.
How often should someone with keratoconus see an eye doctor?
Patients with keratoconus should typically see their eye doctor every 6 to 12 months, depending on the stage and whether the condition is progressing. Younger patients and those with recently diagnosed KC may need more frequent monitoring, sometimes every 3 to 6 months, to watch for progression that may warrant cross-linking.