Arizona's Vision Eye Care Center
LASIK eye surgery corrects nearsightedness, farsightedness, and astigmatism by reshaping the cornea with a laser, and most patients achieve 20/20 vision or better within 24 hours of the procedure. For the thousands of Phoenix residents considering life without glasses or contacts, understanding every stage of the process removes uncertainty and puts you in control of your decision.
This guide walks you through exactly what LASIK is, whether you qualify, how to prepare, what happens in the operating room, and what recovery truly looks like, so you can move forward with clarity and confidence.
What Is LASIK Eye Surgery and How Does It Work?
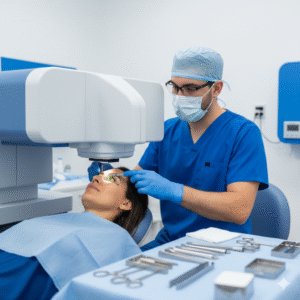
LASIK stands for Laser-Assisted In Situ Keratomileusis. It is a refractive eye surgery that permanently reshapes the cornea, the clear front surface of your eye, so light focuses correctly on the retina. The result is sharper vision without dependence on corrective lenses.
The procedure uses two types of laser technology. First, a femtosecond laser creates a thin, hinged flap in the outer layer of the cornea. Then, an excimer laser removes microscopic amounts of corneal tissue based on your unique prescription map. The flap is repositioned, and it begins healing naturally within minutes. The entire process typically takes less than 15 minutes for both eyes.
LASIK has been FDA-approved since 1999 and has undergone significant technological refinement. Modern wavefront-guided and topography-guided LASIK platforms create customized treatment profiles for each eye, improving precision and visual outcomes beyond what earlier generations of the technology could achieve.
The Science Behind Laser Vision Correction
Your eye works like a camera. The cornea and lens bend (refract) incoming light so it lands precisely on the retina at the back of the eye. When the cornea is too steep, too flat, or irregularly shaped, light focuses in front of or behind the retina, causing blurry vision.
Nearsightedness (myopia) means distant objects appear blurry because the eye is too long or the cornea curves too steeply. Farsightedness (hyperopia) means close objects blur because the eye is too short or the cornea is too flat. Astigmatism results from an irregularly shaped cornea that distorts vision at all distances.
LASIK corrects each of these refractive errors by removing precise amounts of corneal tissue. For myopia, the laser flattens the central cornea. For hyperopia, it steepens the central cornea by removing tissue from the periphery. For astigmatism, it smooths the cornea into a more symmetrical shape. The reshaping is permanent because adult corneal tissue does not regenerate in the treated area.
LASIK vs. Other Vision Correction Procedures
LASIK is the most commonly performed refractive surgery, but it is not the only option. Understanding the alternatives helps you and your eye care provider determine the best fit.
PRK (Photorefractive Keratectomy) removes the outer layer of the cornea (epithelium) entirely instead of creating a flap. It uses the same excimer laser to reshape corneal tissue. PRK is often recommended for patients with thinner corneas who may not be ideal LASIK candidates. Recovery takes longer, typically one to two weeks for functional vision, because the epithelium must regenerate.
SMILE (Small Incision Lenticule Extraction) uses a femtosecond laser to create a small disc of tissue (lenticule) inside the cornea, which the surgeon removes through a tiny incision. There is no flap. SMILE currently treats myopia and astigmatism but is not yet approved for hyperopia.
ICL (Implantable Collamer Lens) involves placing a biocompatible lens inside the eye, in front of the natural lens. It is reversible and suited for patients with very high prescriptions or thin corneas.
Your optometrist can evaluate your corneal thickness, prescription stability, and overall eye health to help determine which procedure aligns with your anatomy and visual goals.
Who Is a Good Candidate for LASIK?
Not everyone qualifies for LASIK. A thorough candidacy evaluation protects your safety and ensures the best possible outcome. The criteria are straightforward, and your eye care provider will assess each one during your consultation.
Age, Prescription, and Eye Health Requirements
Age: You must be at least 18 years old, and most surgeons prefer patients to be 21 or older. The reason is prescription stability. Younger eyes are still changing, and operating on a shifting prescription can lead to under-correction or the need for enhancement surgery.
Stable prescription: Your glasses or contact lens prescription should remain unchanged for at least 12 months before surgery. Significant fluctuations suggest the eye is still developing or responding to hormonal or health changes.
Prescription range: LASIK effectively treats myopia up to approximately -12.00 diopters, hyperopia up to +6.00 diopters, and astigmatism up to 6.00 diopters. Outcomes are most predictable within moderate ranges.
Corneal thickness: The cornea must be thick enough to safely create a flap and allow tissue removal without compromising structural integrity. A minimum corneal thickness of approximately 500 microns is generally required, though this varies by prescription.
General eye health: Candidates should be free of active eye infections, severe dry eye disease, keratoconus (progressive corneal thinning), uncontrolled glaucoma, and significant cataracts. A comprehensive dilated eye exam screens for these conditions.
Overall health: Autoimmune disorders such as lupus or rheumatoid arthritis can impair healing. Uncontrolled diabetes may affect vision stability. Pregnancy and nursing cause temporary prescription changes, so surgery is postponed until hormones stabilize.
Conditions That May Disqualify You from LASIK
Certain findings during your evaluation may rule out LASIK specifically but not necessarily all refractive surgery. These include:
- Corneas that are too thin for safe flap creation (PRK may be an alternative)
- Keratoconus or corneal ectasia, where the cornea is structurally weakened
- Large pupils that exceed the treatment zone, increasing risk of glare and halos
- Severe chronic dry eye that has not responded to treatment
- Previous corneal scarring or certain prior eye surgeries
- Unstable prescriptions that continue to shift year over year
If LASIK is not right for you, your optometrist will explain why and discuss alternatives such as PRK, SMILE, or ICL. A “no” for LASIK does not mean a “no” for clearer vision.
How to Prepare for LASIK Surgery
Preparation begins weeks before your surgery date. Following your provider's instructions closely leads to more accurate measurements, a smoother procedure, and better healing.
Your Pre-Operative Eye Exam and Consultation
The LASIK consultation is more detailed than a standard eye exam. Your eye care provider will perform:
- Corneal topography and tomography to map the shape, curvature, and thickness of your cornea in three dimensions
- Wavefront analysis to measure how light travels through your entire optical system, identifying higher-order aberrations that standard prescriptions do not capture
- Pupil size measurement in dim lighting to assess risk of nighttime visual disturbances
- Tear film evaluation to check for dry eye disease that could affect healing
- Dilated fundus exam to examine the retina and optic nerve for any underlying conditions
- Refraction to confirm your current prescription
These measurements create the treatment profile that guides the laser. Accuracy here directly determines your surgical outcome.
Medications, Contact Lenses, and Lifestyle Adjustments Before Surgery
Contact lens discontinuation is one of the most important pre-operative steps. Contact lenses alter the shape of your cornea temporarily. Soft lenses should be removed at least 5 to 7 days before your evaluation and surgery. Toric soft lenses require 7 to 14 days. Rigid gas permeable (RGP) lenses require 3 to 4 weeks. Your provider will give you a specific timeline.
Medications: Inform your provider about all medications, including over-the-counter drugs and supplements. Some medications affect healing or tear production. You may be asked to start preservative-free artificial tears several times daily in the weeks leading up to surgery to optimize your tear film.
Day of surgery: Do not wear eye makeup, perfume, cologne, or lotions. These products can introduce particles into the surgical environment. Arrange for someone to drive you home, as your vision will be blurry immediately after the procedure.
Questions to Ask Your Eye Care Provider Before LASIK
Walking into your consultation with prepared questions helps you make an informed decision. Consider asking:
- What is my specific prescription, and is it within the ideal LASIK treatment range?
- Is my cornea thick enough for LASIK, or should I consider PRK?
- What technology will be used for my procedure (wavefront-guided, topography-guided, bladeless)?
- What is the surgeon's experience level and complication rate?
- What are the realistic expectations for my vision after surgery?
- How will dry eye be managed before and after the procedure?
- What happens if I need an enhancement or touch-up?
- What does the cost include, and are follow-up visits covered?
Your eye care team should answer every question thoroughly. Feeling rushed or dismissed is a reason to seek a second opinion.
What Happens During the LASIK Procedure?
Understanding the surgical process step by step eliminates the fear of the unknown. LASIK is one of the most studied and refined elective procedures in medicine.
Step-by-Step Breakdown of the Surgery
Step 1: Numbing the eyes. Anesthetic eye drops are applied to both eyes. You will not feel pain during the procedure. A mild oral sedative may be offered to help you relax.
Step 2: Positioning. You lie on a reclining chair beneath the laser system. The surgeon positions your head and places a lid speculum to keep your eyelids open. This feels unusual but is not painful.
Step 3: Creating the corneal flap. The femtosecond laser creates a thin, hinged flap on the surface of the cornea. This takes approximately 10 to 15 seconds per eye. You may feel slight pressure and your vision will temporarily dim or go dark. This is normal.
Step 4: Reshaping the cornea. The surgeon lifts the flap and the excimer laser delivers precisely controlled pulses of ultraviolet light to remove microscopic layers of corneal tissue. The laser is guided by your pre-operative wavefront or topographic map. Modern eye-tracking systems follow your eye movements in real time, pausing if your eye moves out of range. This step takes 20 to 60 seconds depending on your prescription.
Step 5: Repositioning the flap. The surgeon gently places the corneal flap back into position. It adheres naturally without stitches. The flap begins bonding to the underlying tissue within minutes.
Step 6: Immediate post-operative check. The surgeon examines the flap position under a microscope. You rest briefly, then receive post-operative eye drops and protective shields.
Total time in the laser suite is typically 15 to 20 minutes for both eyes. The actual laser treatment per eye lasts under a minute.
What You Will See, Feel, and Hear During LASIK
Knowing what your senses will experience prevents surprise and anxiety.
Vision: You will see a blinking fixation light that you focus on throughout the procedure. When the femtosecond laser activates, your vision may go gray or dark for several seconds. This is expected. During the excimer laser phase, you will see the blinking light through a slightly blurry field.
Sensation: The numbing drops eliminate pain. You will feel the lid speculum holding your eye open and mild pressure during flap creation. Some patients describe a sensation of coolness during the excimer laser phase. There is no sharp or stinging pain.
Sound: The excimer laser produces a quiet clicking or buzzing sound. Some patients notice a faint smell, similar to something burning. This is the byproduct of the laser vaporizing corneal tissue at a molecular level and is completely normal.
Duration awareness: Because the procedure is so fast, most patients report that it was over before they had time to feel nervous.
LASIK Recovery: What to Expect After Surgery
Recovery from LASIK is faster than most patients anticipate, but following your post-operative care plan is essential for optimal healing and visual results.
The First 24 to 48 Hours After LASIK
Immediately after surgery, your vision will be hazy, similar to looking through a foggy window. Most patients notice significant improvement within 2 to 4 hours. By the next morning, many can see well enough to drive, though you should confirm this at your one-day follow-up appointment.
Common experiences in the first 24 to 48 hours include:
- Mild burning, tearing, or a gritty sensation (typically resolves within 4 to 6 hours)
- Light sensitivity (wear the provided sunglasses, even indoors if needed)
- Watery eyes
- Slight fluctuation in vision clarity
You will be instructed to sleep with protective eye shields for the first several nights to prevent accidental rubbing. Rest and keep your eyes closed as much as possible on the day of surgery. Avoid screens for the first 24 hours if possible.
Week-by-Week Recovery Timeline
Week 1: Most patients return to work and normal activities within 1 to 2 days. Vision continues to sharpen. Mild dryness and intermittent blurriness are common. Use prescribed artificial tears frequently. Avoid rubbing your eyes, swimming, hot tubs, and dusty environments.
Weeks 2 to 4: Vision stabilizes for the majority of patients. Dry eye symptoms typically peak around week 2 and then gradually improve. Nighttime glare and halos around lights may be noticeable but usually diminish over this period. You can resume exercise, though avoid contact sports and wear protective eyewear.
Months 1 to 3: Residual dryness continues to improve. Any remaining visual fluctuations typically resolve. Your eye care provider will monitor your healing at scheduled follow-up visits.
Months 3 to 6: Vision reaches its final stable outcome for most patients. Dry eye symptoms have resolved for the majority. Your provider will perform a comprehensive post-operative exam to confirm your results and update your records.
Post-Operative Care Instructions and Follow-Up Visits
Your post-operative regimen typically includes:
- Antibiotic eye drops for 5 to 7 days to prevent infection
- Anti-inflammatory steroid eye drops for 1 to 4 weeks to control healing response
- Preservative-free artificial tears used liberally for at least 1 to 3 months, and longer if dryness persists
Follow-up visits are usually scheduled at 1 day, 1 week, 1 month, 3 months, and 6 months after surgery. These appointments allow your eye care provider to monitor flap healing, measure your vision, check eye pressure (steroid drops can temporarily raise intraocular pressure), and manage any dry eye symptoms.
Do not skip follow-up appointments. Early detection of any healing irregularity leads to faster and simpler correction.
LASIK Results, Risks, and Side Effects
LASIK has one of the highest patient satisfaction rates of any elective procedure. Understanding realistic outcomes and potential risks helps you set appropriate expectations.
Typical Vision Outcomes and Success Rates
According to the American Academy of Ophthalmology, more than 90% of LASIK patients achieve 20/20 vision or better, and over 99% achieve 20/40 or better, which is the legal standard for driving without corrective lenses in most states.
A comprehensive review published in the Journal of Cataract & Refractive Surgery found that over 96% of patients reported satisfaction with their LASIK results. This places LASIK among the highest-satisfaction elective procedures in all of medicine.
Most patients notice dramatically improved vision within hours. Final visual acuity stabilizes over 3 to 6 months as the cornea completes its healing process.
It is important to understand that LASIK corrects your current prescription. It does not prevent age-related changes. Presbyopia, the gradual loss of near focusing ability that typically begins in the mid-40s, will still occur. You may eventually need reading glasses even after successful LASIK.
Common Side Effects and How Long They Last
Most side effects are temporary and resolve within the first 1 to 3 months:
- Dry eyes: The most common side effect. The flap creation temporarily disrupts corneal nerves that signal tear production. Frequent artificial tear use manages symptoms. Most patients experience significant improvement by month 3.
- Glare and halos: Rings or starbursts around lights, especially at night. More common in patients with large pupils or high prescriptions. Typically diminishes within 1 to 3 months.
- Light sensitivity: Usually resolves within the first week.
- Minor visual fluctuations: Slight blurriness that comes and goes during the healing period. Stabilizes within weeks to months.
Rare Complications and When to Contact Your Doctor
Serious complications are uncommon but possible. Being informed allows you to respond quickly.
- Flap complications: Wrinkles, displacement, or incomplete flaps occur in a small percentage of cases. Most are identified and corrected during surgery or at the first follow-up visit.
- Infection: Extremely rare with proper antibiotic drop use. Symptoms include increasing pain, redness, and worsening vision after the first day.
- Ectasia: Progressive corneal thinning and bulging that can occur months or years after surgery. Thorough pre-operative screening for keratoconus and adequate corneal thickness significantly reduces this risk.
- Diffuse lamellar keratitis (DLK): An inflammatory reaction under the flap, sometimes called “sands of the Sahara.” Detected at follow-up visits and treated with increased steroid drops.
- Regression: A gradual return of some refractive error over time. Enhancement surgery can address this if the cornea has sufficient remaining thickness.
Contact your eye care provider immediately if you experience: sudden vision loss, severe pain that worsens after the first day, significant increase in redness, or any discharge from the eye.
How Much Does LASIK Cost in Phoenix, AZ?
Cost is one of the most common concerns for patients considering LASIK. Understanding what drives pricing helps you evaluate quotes and avoid surprises.
Factors That Affect LASIK Pricing
In the Phoenix metropolitan area, LASIK typically ranges from $1,500 to $3,000 per eye, depending on several factors:
- Technology used: Bladeless, wavefront-guided, and topography-guided platforms cost more than older microkeratome-based systems but offer greater precision and customization.
- Surgeon experience: Surgeons with extensive refractive surgery experience and strong track records may charge higher fees.
- Prescription complexity: Higher prescriptions or significant astigmatism may require more advanced treatment profiles.
- Included services: Some quotes are all-inclusive (pre-operative exams, surgery, all follow-up visits, enhancement coverage), while others charge separately for each component. Always ask what is included.
Be cautious of heavily discounted advertising. Extremely low prices may indicate older technology, less experienced surgeons, or fees that exclude essential components like follow-up care.
Insurance, Financing, and FSA/HSA Options
Most vision and medical insurance plans classify LASIK as an elective procedure and do not cover it. However, several financial options make LASIK accessible:
- FSA (Flexible Spending Account) and HSA (Health Savings Account): LASIK is an eligible expense. You can use pre-tax dollars, effectively reducing the cost by your tax rate.
- Financing plans: Many LASIK centers offer interest-free or low-interest payment plans through medical financing companies like CareCredit or Alphaeon Credit.
- Employer vision benefits: Some employers offer LASIK discounts through preferred provider networks. Check with your HR department.
- Lifetime enhancement policies: Some providers include free or discounted enhancement surgery if your vision changes after the initial procedure. This adds long-term value to the investment.
When comparing costs, calculate the long-term savings. The average contact lens wearer spends $500 to $800 per year on lenses, solution, and related eye exams. Over 10 to 20 years, LASIK often pays for itself.
The Role of Your Optometrist in LASIK Eye Surgery
Many patients are surprised to learn that their optometrist plays a central role in the LASIK process. Understanding how optometrists and ophthalmologists collaborate ensures you receive coordinated, comprehensive care.
How Optometrists and Ophthalmologists Work Together for LASIK
Optometrists and ophthalmologists are both licensed eye care professionals, but their training and scope of practice differ.
Optometrists complete a Doctor of Optometry (O.D.) degree and specialize in comprehensive eye exams, vision correction, diagnosis and management of many eye conditions, and pre- and post-operative care for eye surgeries including LASIK. They are your primary eye care providers.
Ophthalmologists complete medical school (M.D. or D.O.) followed by a residency in ophthalmology. They perform eye surgeries, including LASIK, and manage complex medical and surgical eye conditions.
In the LASIK care pathway, these professionals work as a team:
- Your optometrist performs the initial comprehensive evaluation, determines candidacy, takes pre-operative measurements, and refers you to a trusted ophthalmologist/refractive surgeon.
- The ophthalmologist/refractive surgeon performs the LASIK procedure.
- Your optometrist manages all post-operative follow-up care, monitoring healing, managing dry eye, tracking visual outcomes, and addressing any concerns.
This co-management model is the standard of care in refractive surgery. It means you receive the specialized surgical expertise of an ophthalmologist combined with the ongoing, accessible care of your local optometrist.
Why Your Eye Care Team Matters Before and After Surgery
The quality of your pre-operative evaluation directly affects your surgical outcome. Accurate corneal measurements, thorough screening for disqualifying conditions, and honest candidacy assessment protect you from complications.
Post-operative care is equally critical. Your optometrist monitors healing at multiple intervals, adjusts medications, manages dry eye, and catches any irregularities early when they are most treatable. Having a local provider you trust and can reach easily makes the recovery process smoother and less stressful.
Choosing a LASIK pathway that includes coordinated optometric and ophthalmologic care is not just convenient. It is a clinical best practice that improves outcomes and patient satisfaction.
Choosing the Right LASIK Provider in Phoenix, AZ
The decision of where to have LASIK is as important as the decision to have it. Not all providers offer the same technology, experience, or level of care.
What to Look for in a LASIK Surgeon and Eye Care Center
When evaluating LASIK providers in the Phoenix area, prioritize:
- Surgeon credentials and volume: Look for a board-certified ophthalmologist with fellowship training or extensive experience in refractive surgery. Surgeons who perform a high volume of LASIK procedures maintain sharper skills and encounter a wider range of cases.
- Technology: Ask about the specific laser platforms used. Current-generation femtosecond lasers for flap creation and wavefront-guided or topography-guided excimer lasers for corneal reshaping represent the standard of care.
- Comprehensive candidacy screening: Providers who take time for thorough evaluations, including corneal topography, tomography, tear film analysis, and dilated exams, prioritize your safety over surgical volume.
- Transparent pricing: All-inclusive pricing that covers pre-operative exams, surgery, follow-up visits, and enhancement policies eliminates hidden costs.
- Co-management relationships: A strong partnership between the surgical center and your referring optometrist ensures continuity of care.
- Patient reviews and outcomes data: Ask about the center's reported outcomes and read patient testimonials specific to LASIK.
How Arizona's Vision Eye Care Center Supports Your LASIK Journey
At Arizona's Vision Eye Care Center, we guide Phoenix-area patients through every phase of the LASIK process. Our role begins with a comprehensive LASIK candidacy evaluation using advanced diagnostic technology to determine whether LASIK, PRK, or another option is the best fit for your eyes.
We partner with experienced, board-certified refractive surgeons in the Phoenix area and coordinate your care from initial consultation through final post-operative visit. Our optometrists manage your pre-operative preparation, ensure your measurements are precise, and handle all follow-up care after surgery.
If LASIK is not the right choice for your eyes, we explain why and present alternatives. Our priority is your long-term eye health and visual satisfaction, not a surgical referral. That commitment to honest, patient-centered guidance is what sets our approach apart.
Conclusion
LASIK eye surgery is a well-established, highly effective procedure that corrects nearsightedness, farsightedness, and astigmatism by reshaping the cornea with laser precision. Understanding candidacy requirements, preparation steps, the surgical process, and realistic recovery expectations empowers you to make a confident, informed decision about your vision.
The right outcome depends not only on the surgery itself but on the quality of care surrounding it. From thorough pre-operative screening to attentive post-operative management, every step in the LASIK journey matters, and the partnership between your optometrist and surgeon is what ties it all together.
At Arizona's Vision Eye Care Center, we are here to walk you through every stage, answer every question, and ensure you receive the right care at the right time. If you are considering LASIK in Phoenix, schedule your candidacy evaluation with our team today and take the first step toward clearer vision.
Frequently Asked Questions About LASIK Eye Surgery
How do I know if I am a good candidate for LASIK?
You may be a good candidate if you are at least 18 years old, have a stable prescription for at least 12 months, and have healthy corneas with adequate thickness. A comprehensive LASIK evaluation with your optometrist is the only way to confirm candidacy, as it includes corneal mapping, tear film analysis, and a full eye health assessment.
Does LASIK hurt?
No. Numbing eye drops are applied before the procedure, so you will not feel pain during surgery. Most patients experience mild burning, tearing, or a gritty sensation for a few hours afterward, which resolves quickly. The procedure itself takes less than a minute of laser time per eye.
How long does it take to recover from LASIK?
Most patients see well enough to return to work and daily activities within 1 to 2 days. Vision continues to sharpen over the first week, and full stabilization typically occurs within 3 to 6 months. Dry eye symptoms and nighttime glare usually improve steadily during this period.
Can LASIK fix astigmatism?
Yes. LASIK effectively corrects astigmatism by reshaping the irregular curvature of the cornea into a more symmetrical shape. Modern wavefront-guided and topography-guided laser platforms treat astigmatism with high precision, and it is one of the most common refractive errors addressed during LASIK.
What is the difference between LASIK and PRK?
Both procedures use an excimer laser to reshape the cornea. The key difference is how the corneal surface is accessed. LASIK creates a thin flap that is lifted and repositioned. PRK removes the outer layer of the cornea entirely, which then regenerates during healing. PRK has a longer recovery period but may be recommended for patients with thinner corneas.
Will I still need glasses after LASIK?
Most patients achieve 20/20 vision or better and no longer need glasses for distance vision. However, LASIK does not prevent presbyopia, the age-related loss of near focusing ability that typically begins in your mid-40s. You may eventually need reading glasses for close-up tasks regardless of LASIK.
Why does my optometrist handle my LASIK follow-up care instead of the surgeon?
Co-management is the standard of care in refractive surgery. Your optometrist is trained to monitor post-operative healing, manage dry eye, track visual outcomes, and detect any complications early. Because your optometrist is local and accessible, this model provides more convenient, consistent follow-up care while keeping the surgeon available for any surgical concerns that may arise.